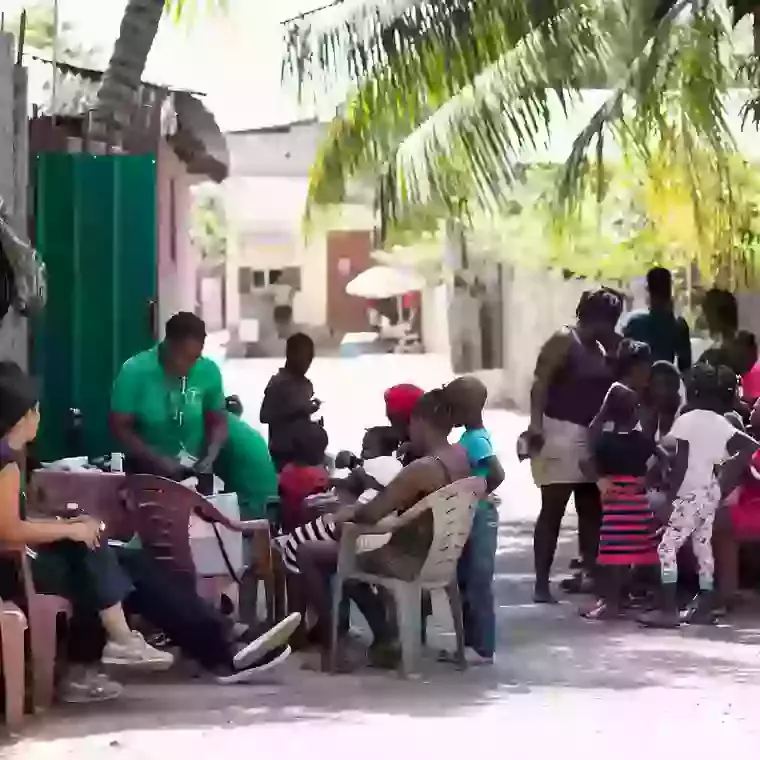Supporting a vast range of maternity services, ensuring the world’s poorest have access to life-saving healthcare.
Haiti:
99% of maternal deaths happen in the developing world, most from avoidable complications. Haiti has the highest rate of maternal mortality in the western hemisphere, with 63% of deliveries taking place at home, without any formal medical support. We support the running and development of community health programmes and a leading hospital in North Haiti, which employs 270 Haitian staff and treats over 20,000 patients a year.
Maternal Care:
HHA believe every mother and baby deserve the right to life, with the help of safe and dignified maternal health. Each year we support thousands of women through a range of community and hospital-based activities, as we fight to reduce maternal mortalities globally.
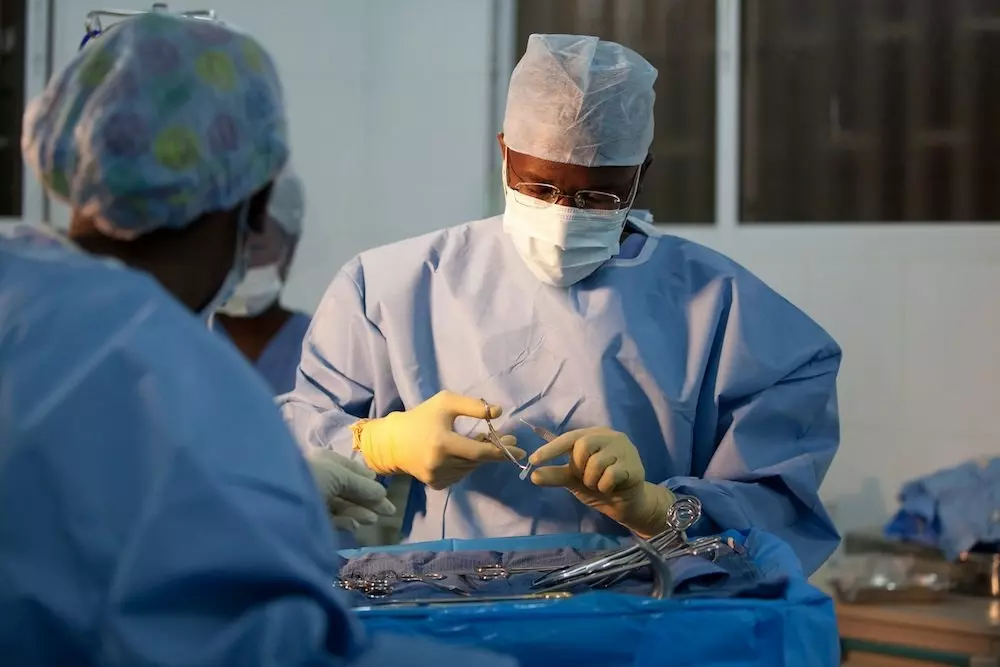
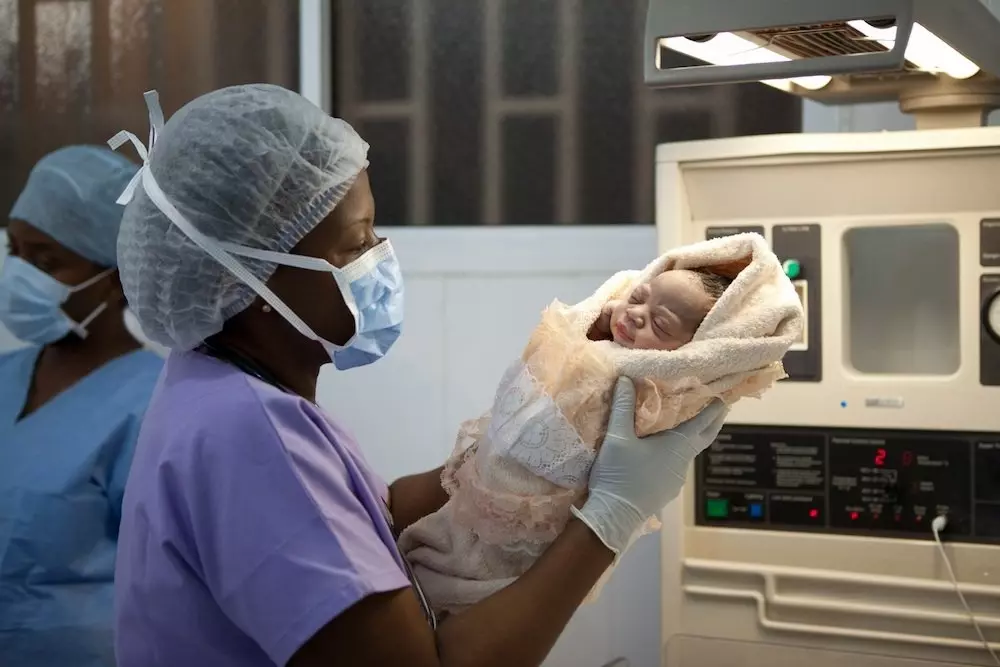
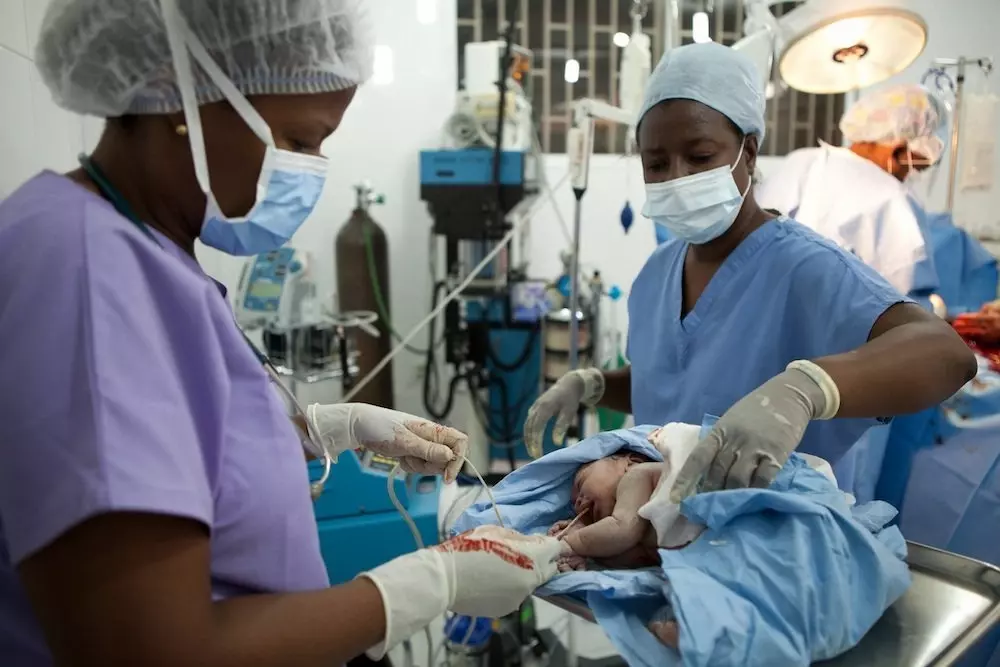
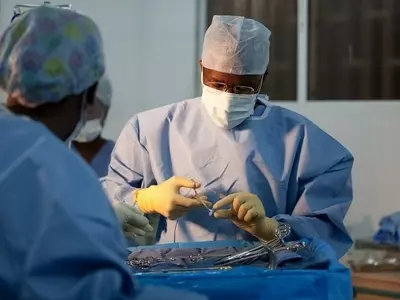
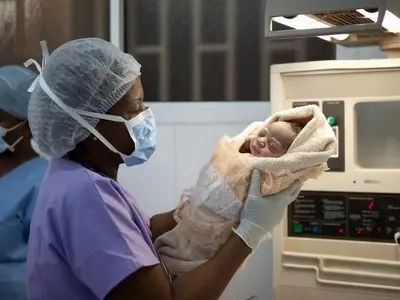
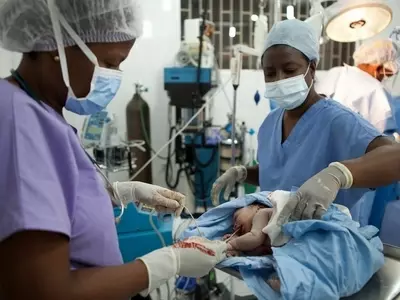
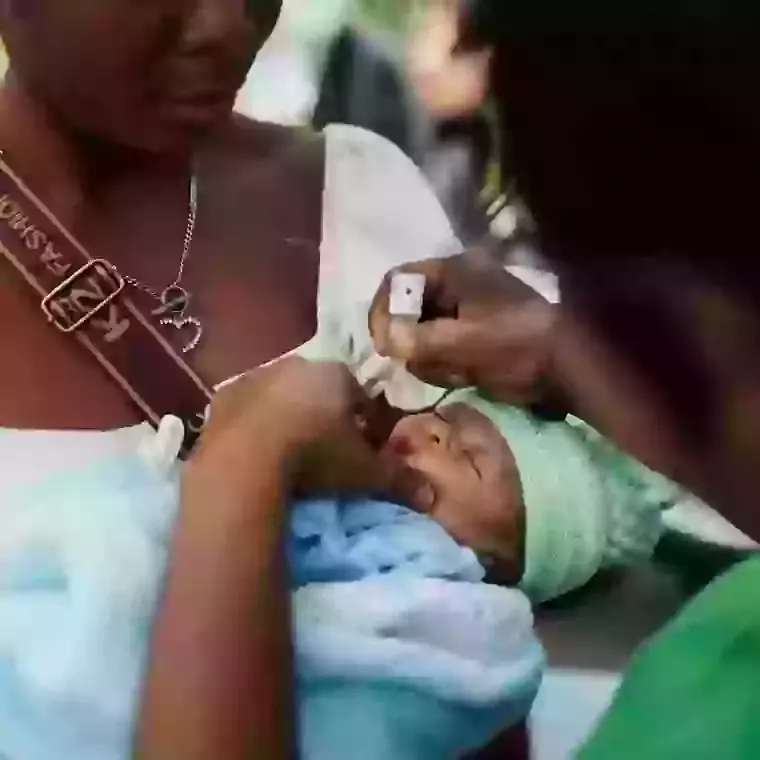
We support one of North Haiti’s leading Maternity Units, a 25-bed facility that provides 24/7obstetrical care, with two natural birthing suites and an emergency obstetrical operating theatre. Between July 2016 – June 2017 this unit provided 1,592 deliveries, of which over 33% were emergency C-Sections, providing lifesaving, hospital-based care to some of Haiti’s poorest women. The facility also provided thousands of other consultations, including 3,539 antenatal appointments.
We also worked with Kings College London (KCL) on a 3-year trial called CRADLE. This project introduced a newly developed blood pressure device into three of Cap-Haitien’s leading maternity facilities, to help detect high risk maternal cases more swiftly. Following on from this great work we’re delighted to be partnering with KCL on two other exciting projects, including launching the CRADLE device in Bidibidi Refugee Settlement, Uganda, (the largest in the world). In 2018 we worked with over 470 Volunteer Health Teams and 17+ UNHCR Health Facilities on this project.
Project Start Date: 2012
Safe births: 1600+ births supported each year
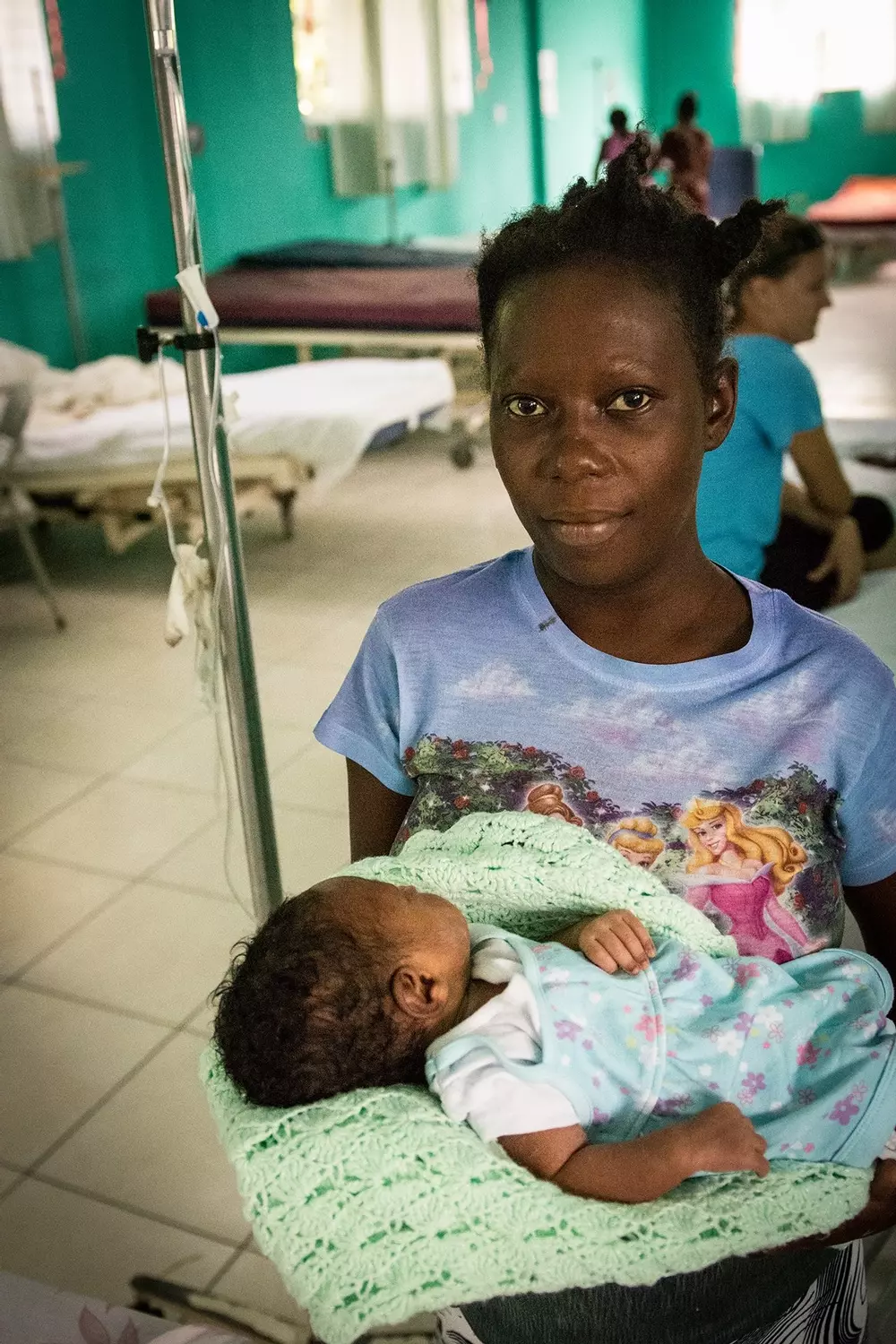
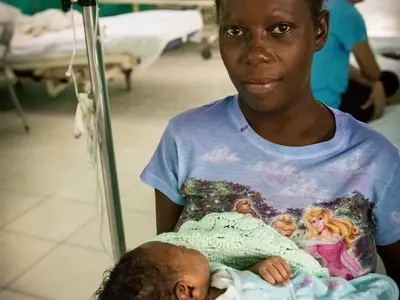
Haiti Maternity Case Study
Davilma lives around 40 minutes from our hospital and recently gave birth to her 3rd child, prematurely, at just 31 weeks. This is Davilma’s story:
‘At my prenatal visit, the doctor was doing an ultra-sound and she noticed something strange so she asked me how I was feeling. I said I've been having lower stomach pains frequently so the doctor said I would need to stay at hospital. I gave birth at 7 months and one week, which means my child is premature.’
As well as the baby being premature, Davilma also faced a fight for survival during the birth: ‘I almost died as well, I lost a lot of blood.’
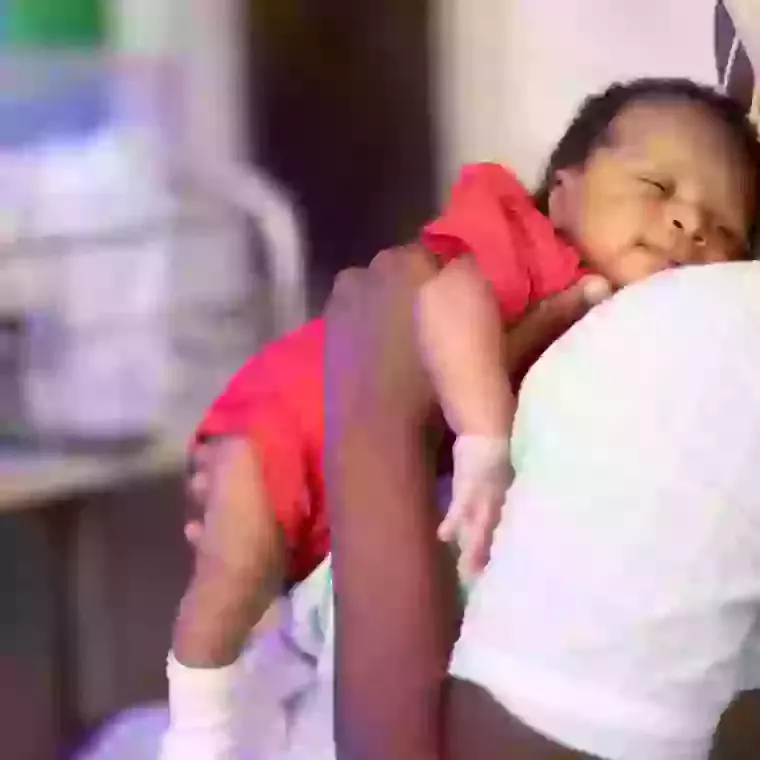
Davilma’s baby boy was small and weak, and the doctors were not confident he would survive. But through the excellent care of the Neonatal staff, Davilma’s prayers were answered. Her baby is responding to treatment and is feeding well. He has a positive future ahead. ‘I feel proud and joyful that my child is alive and doing well...'
Davilma knows that she probably would not have survived had she given birth at home. Maintaining and growing the maternity and neonatal services at our partner hospital is more important than ever.